Pelvic fracture rehabilitation centers on a biopsychosocial model‚ guided by the ICF framework‚ aiming to optimize outcomes and minimize lasting disabilities.
Effective rehabilitation protocols‚ whether nonoperative or post-surgical‚ are crucial for restoring function and improving the patient’s overall health.
Initial management often involves immobilization with braces or casts‚ alongside tailored strategies for pain control and complication prevention.
Understanding Pelvic Fractures
Pelvic fractures encompass a spectrum of injuries‚ ranging from stable‚ minimally displaced breaks to unstable‚ complex disruptions requiring surgical intervention.
Fragility fractures‚ common in the elderly‚ often present insidiously‚ while high-energy trauma typically causes more severe damage. Accurate classification is vital for guiding treatment.
Rehabilitation protocols must consider fracture type‚ patient stability‚ and associated injuries‚ prioritizing early mobilization when medically appropriate to prevent secondary complications.
Importance of a Rehabilitation Protocol
A structured rehabilitation protocol is paramount following a pelvic fracture‚ aiming to maximize functional recovery and minimize long-term disability.
Integrative approaches‚ guided by the biopsychosocial model and ICF framework‚ address physical‚ psychological‚ and social needs.
Early‚ progressive exercise‚ coupled with appropriate assistive device training‚ optimizes healing‚ restores mobility‚ and facilitates a return to meaningful activity.

Initial Assessment and Patient Evaluation
Comprehensive evaluation includes medical history‚ fracture classification‚ and detailed neurological and musculoskeletal examinations to tailor rehabilitation.
Determining stability and associated injuries guides treatment decisions and informs the development of an individualized rehabilitation plan.
Medical History and Fracture Classification
Detailed medical history reveals comorbidities impacting healing‚ like osteoporosis in fragility fractures. Fracture classification—stable vs. unstable—dictates treatment.
Insidious onset characterizes pelvic insufficiency fractures in the elderly‚ requiring careful assessment. Understanding fracture patterns (e.g.‚ transverse‚ oblique) informs rehabilitation intensity and precautions.
Prior surgeries and medications are noted‚ influencing the rehabilitation protocol and potential complications.
Neurological and Musculoskeletal Examination
Neurological assessment checks for nerve damage impacting lower limb function‚ sensation‚ and bowel/bladder control. Musculoskeletal evaluation assesses range of motion‚ muscle strength‚ and pain levels around the pelvis and lower extremities.
Palpation identifies tenderness and instability. Gait analysis reveals impairments. These findings guide rehabilitation‚ tailoring exercises to address specific deficits and prevent further injury.
Documenting pre-injury function establishes a baseline for measuring progress.
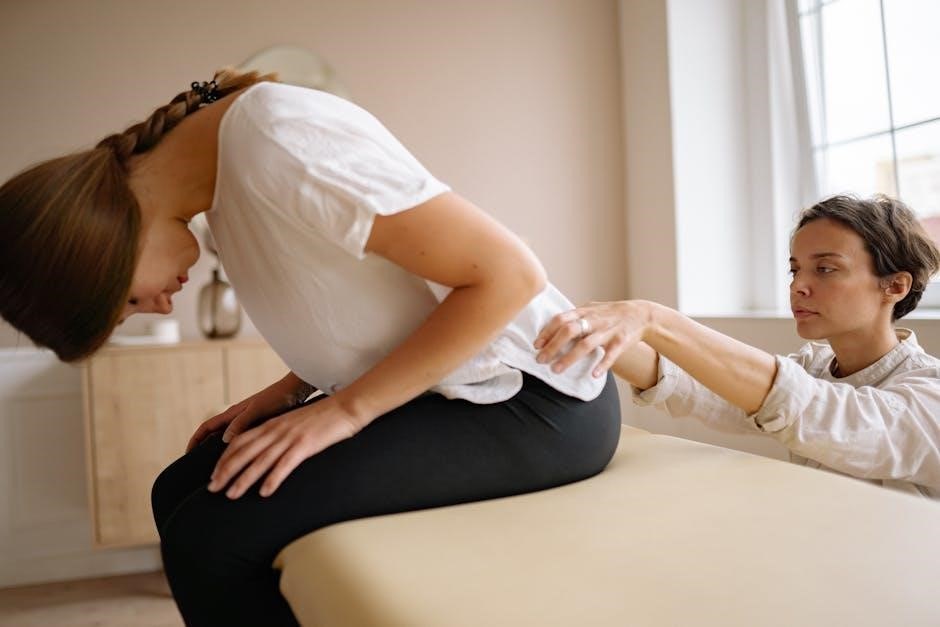
Acute Phase Management (0-6 Weeks)
Initial care prioritizes pain control‚ immobilization via braces or casts‚ and preventing complications like DVTs.
Wound care is essential post-surgery‚ while careful monitoring for neurological deficits is paramount during this early stage.
Immobilization Techniques: Braces and Casts
Immobilization‚ utilizing braces or casts‚ is fundamental in the acute phase‚ ensuring pelvic bone stabilization and preventing further injury.
The choice depends on fracture stability; braces allow some movement while providing support‚ whereas casts offer rigid immobilization.
Regular skin checks are vital to prevent pressure sores‚ and patient education on proper brace/cast care is essential for optimal healing.
Pain Management Strategies
Effective pain management is paramount throughout pelvic fracture rehabilitation‚ significantly impacting patient participation and recovery.
Strategies include pharmacological interventions – analgesics‚ nerve blocks – alongside non-pharmacological approaches like ice‚ positioning‚ and relaxation techniques.
A multidisciplinary approach‚ addressing both physical and psychological aspects of pain‚ optimizes comfort and functional progress.
Preventing Complications: DVT Prophylaxis & Wound Care
Proactive complication prevention is vital during pelvic fracture rehabilitation. DVT prophylaxis‚ utilizing pharmacological and mechanical methods‚ minimizes thromboembolic risk.
Meticulous wound care‚ monitoring for infection‚ and appropriate dressing changes are essential‚ particularly post-surgery.
Early mobilization‚ when appropriate‚ further reduces DVT risk and promotes healing‚ contributing to a smoother recovery trajectory.
Early Rehabilitation Phase (6-12 Weeks)
Gentle range of motion exercises and isometric strengthening initiate recovery. Assistive devices‚ like crutches‚ facilitate safe mobility and weight-bearing progression.
Focus remains on pain management and establishing a foundation for more advanced rehabilitation.
Gentle Range of Motion Exercises
Early mobilization with gentle range of motion (ROM) exercises is paramount‚ focusing on pain-free movements. Ankle pumps‚ hip and knee bends‚ and gentle trunk rotations are initiated.
These exercises combat stiffness‚ maintain joint lubrication‚ and prevent muscle atrophy. Progression is guided by pain levels and fracture stability‚ avoiding excessive stress.
The goal is to restore basic movement patterns and prepare the patient for more demanding activities in subsequent phases of rehabilitation.
Isometric Exercises for Pelvic Stabilization
Isometric exercises are introduced to activate pelvic and core musculature without joint movement‚ enhancing pelvic stabilization. These include gluteal sets‚ abdominal bracing‚ and adductor squeezes.
Focus is on maintaining muscle engagement for several seconds‚ gradually increasing hold times. This builds a foundation of strength and control‚ crucial for functional recovery.
Isometric contractions minimize stress on the fracture site while promoting neuromuscular re-education and preparing for dynamic exercises.
Assistive Device Training: Crutches or Walkers
Assistive devices‚ such as crutches or walkers‚ are essential for early mobilization while protecting the healing fracture. Proper fitting and gait training are paramount to ensure safety and prevent compensatory movements.
Patients learn weight-bearing precautions and techniques for navigating various surfaces. Progressive weaning from the device occurs as strength and stability improve.
The goal is to restore a normal gait pattern and functional independence‚ minimizing the risk of falls and promoting confidence in movement.
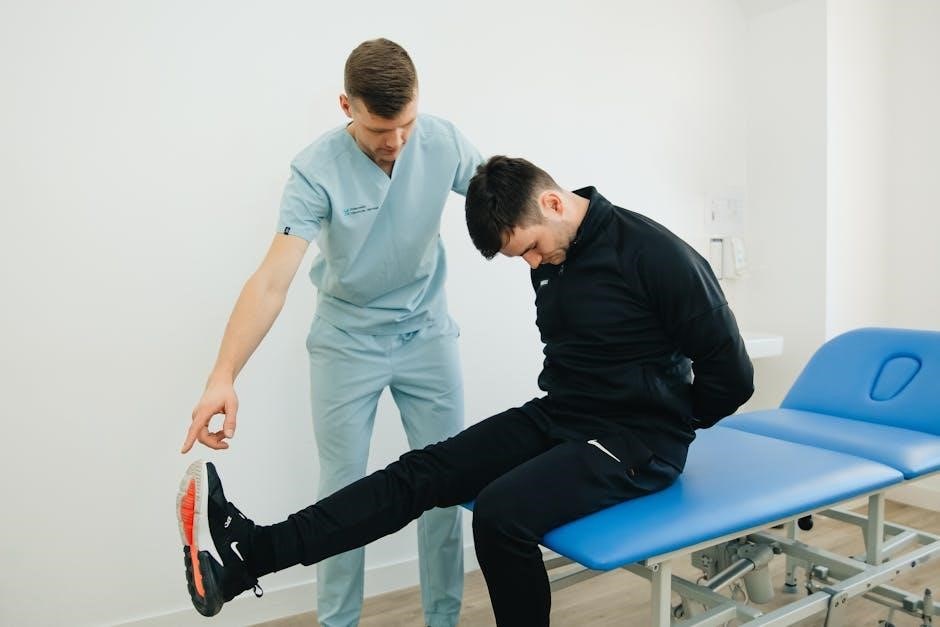
Intermediate Rehabilitation Phase (12-18 Weeks)
Progressive strengthening‚ gait training‚ and core stabilization are key during this phase. Healing timeframes post-surgery typically fall within this period.
Focus shifts towards functional movements and improving balance‚ preparing patients for more demanding activities.
Progressive Strengthening Exercises
Strengthening begins with isometric exercises‚ gradually progressing to resistance bands and light weights. Hip abductors‚ adductors‚ and extensors are targeted to rebuild pelvic stability.
Exercises like bridging‚ clamshells‚ and side leg raises are incorporated. Careful monitoring prevents overload‚ ensuring fracture healing isn’t compromised. Progression is guided by pain levels and radiographic assessment.
Focus remains on controlled movements‚ avoiding sudden impacts or twisting motions that could jeopardize the fracture site.
Gait Training and Balance Exercises
Gait training progresses from assistive devices – crutches or walkers – to independent ambulation‚ focusing on symmetrical weight-bearing. Balance exercises‚ like single-leg stance and tandem walking‚ are introduced cautiously.
Proprioceptive awareness is enhanced through exercises on unstable surfaces. The goal is to restore a normal gait pattern and minimize fall risk‚ crucial for long-term function.
Regular assessment ensures safety and appropriate progression‚ adapting to individual patient needs.
Core Stabilization Exercises
Core stabilization is paramount‚ initiating with gentle abdominal bracing and progressing to exercises targeting the transverse abdominis‚ multifidus‚ and pelvic floor muscles.
These exercises enhance pelvic control and spinal stability‚ reducing stress on the fracture site. Isometric exercises are foundational‚ followed by dynamic movements.
A strong core supports functional activities and prevents compensatory movement patterns‚ aiding in a full recovery.
Advanced Rehabilitation Phase (18+ Weeks)
Functional exercises and proprioceptive training restore activity-specific movements and balance. Imaging monitors healing‚ ensuring safe progression towards full return to function.
Functional Exercises and Return to Activity
Functional exercises progressively challenge patients with real-world tasks‚ bridging the gap between rehabilitation and daily life. These include stair climbing‚ walking varied terrains‚ and simulated work activities.
Return to activity is gradual and individualized‚ guided by pain levels and functional assessments. The goal is to regain independence and participation in desired activities‚ optimizing quality of life.
Careful monitoring ensures a safe and effective transition back to pre-injury levels of function.
Proprioceptive Training
Proprioceptive training focuses on restoring the patient’s awareness of their pelvic position and movement in space‚ crucial for balance and coordination.
Exercises involve unstable surfaces‚ single-leg stance‚ and dynamic movements‚ challenging the neuromuscular system to regain control. This minimizes fall risk and enhances functional stability.
Improved proprioception supports a safe and confident return to activity.
Monitoring Healing Progress with Imaging
Radiological assessment‚ particularly conventional radiology‚ remains vital for tracking fracture healing throughout rehabilitation.
Regular imaging allows clinicians to evaluate callus formation‚ bone alignment‚ and identify potential complications like non-union.
Healing timelines post-surgery typically range from 12 to 18 weeks‚ guided by imaging findings and clinical progress.
Surgical vs. Non-Operative Rehabilitation Approaches
Rehabilitation is tailored to the treatment path – nonoperative care‚ sacroplasty‚ or internal fixation – influencing timelines and exercise progression.
Post-surgical healing generally requires a more cautious and phased approach compared to non-operative management.
Tailoring Rehabilitation to Treatment Type
Rehabilitation protocols must be individualized‚ considering whether the pelvic fracture was managed surgically or non-operatively.
Surgical interventions‚ like iliosacral screw fixation‚ necessitate a more gradual progression‚ prioritizing wound healing and hardware stabilization before loading.
Non-operative approaches emphasize early mobilization within pain limits‚ focusing on muscle activation and preventing secondary complications like stiffness.
The ICF framework guides a holistic approach‚ addressing functional limitations specific to each treatment pathway.
Healing Timeframes Post-Surgery
Post-surgical healing of pelvic fractures typically spans 12 to 18 weeks‚ though individual timelines vary based on fracture complexity and patient factors.
Early phases (0-6 weeks) prioritize pain management and protected weight-bearing‚ utilizing braces or casts for stabilization.
Progressive loading and strengthening commence around 6-12 weeks‚ guided by radiographic evidence of callus formation and bone healing.
Full functional recovery may extend beyond 6 months‚ requiring continued rehabilitation and monitoring.
Considerations for Fragility Fractures in the Elderly
Fragility fractures require addressing co-morbidities and implementing fall prevention strategies alongside rehabilitation to optimize recovery and minimize future risk.
Care must be individualized‚ considering reduced physiological reserves and potential for slower healing processes.
Addressing Co-morbidities
Elderly patients frequently present with pre-existing conditions like osteoporosis‚ cardiovascular disease‚ or diabetes‚ significantly impacting pelvic fracture rehabilitation.
A comprehensive assessment is vital to manage these co-morbidities concurrently‚ optimizing medical stability before initiating intensive therapy.
Medication management‚ nutritional support‚ and careful monitoring are essential for safe and effective rehabilitation progress.
Fall Prevention Strategies
Fragility fractures in the elderly often result from falls; therefore‚ fall prevention is paramount during and after pelvic fracture rehabilitation.
Strategies include home hazard assessments‚ modification of the living environment‚ and balance/strength training to improve stability.
Vision checks‚ medication reviews‚ and addressing underlying medical conditions are also crucial components of a comprehensive prevention plan.

Role of the Biopsychosocial Model in Rehabilitation
Rehabilitation benefits from a biopsychosocial approach‚ addressing psychological impact and social support alongside physical recovery‚ guided by the ICF framework.
This holistic model improves outcomes and facilitates a successful return to work and daily activities post-fracture.
Addressing Psychological Impact
Pelvic fractures can induce significant psychological distress‚ including anxiety‚ depression‚ and fear of movement‚ impacting rehabilitation adherence.
A biopsychosocial approach necessitates screening for these issues and providing appropriate interventions like counseling or cognitive behavioral therapy.
Acknowledging emotional challenges fosters patient engagement and optimizes functional recovery‚ improving overall well-being throughout the rehabilitation process.
Social Support and Return to Work
Robust social support networks are vital for successful pelvic fracture rehabilitation‚ aiding emotional well-being and adherence to treatment plans.
Facilitating a safe return to work requires a graded approach‚ considering physical demands and potential workplace modifications.
Collaboration with employers and vocational rehabilitation specialists ensures a sustainable and fulfilling reintegration into professional life post-injury.
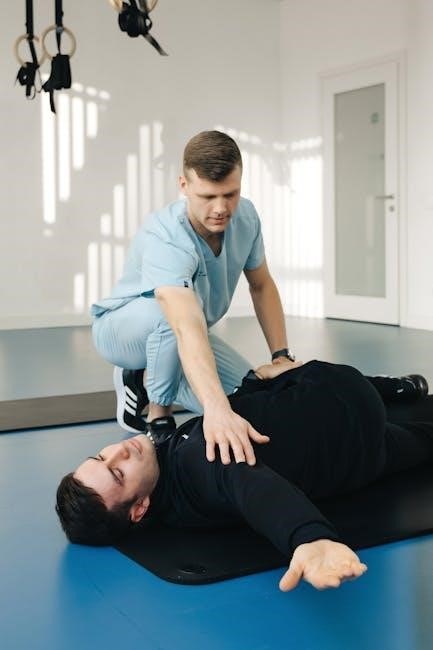
Transfer Protocols and Hospital Discharge Planning
Patients with suspected pelvic fractures should be transferred to a general hospital‚ or a Major Trauma Centre if unstable.
Discharge planning includes a tailored home exercise program‚ ensuring continued progress and minimizing complications post-hospitalization.
Criteria for Transfer to Major Trauma Centers
Haemodynamically unstable patients‚ or those with polytrauma alongside a pelvic fracture‚ necessitate immediate transfer to a Major Trauma Centre (MTC).
If direct transfer isn’t feasible‚ initial resuscitation at a trauma unit is vital‚ followed by prompt relocation to an MTC. This ensures access to specialized surgical and rehabilitative expertise.
Rapid assessment and adherence to established protocols are paramount for optimizing patient outcomes in complex pelvic fracture cases.
Home Exercise Program Development
A tailored home exercise program is essential for continued progress post-discharge‚ focusing on gentle range of motion and isometric pelvic stabilization exercises.
Programs should be individualized‚ considering fracture stability and patient tolerance‚ and progressively increase in intensity. Clear instructions and demonstration are crucial.
Regular monitoring and adjustments by a physical therapist ensure safety and maximize functional recovery within the rehabilitation protocol.
Utilizing the International Classification of Functioning‚ Disability and Health (ICF) Framework
The ICF framework guides a holistic approach‚ addressing biological‚ psychological‚ and social factors impacting function after a pelvic fracture.
This ensures patient-centered care‚ optimizing rehabilitation by considering individual needs and environmental influences.
Applying ICF Principles to Pelvic Fracture Rehabilitation
Applying ICF principles necessitates a comprehensive assessment beyond impairment‚ evaluating activity limitations and participation restrictions post-fracture.
Rehabilitation goals should target all ICF domains – body functions‚ activities‚ and participation – considering environmental and personal factors.
This integrative approach‚ guided by the ICF‚ improves outcomes and reduces residual disabilities‚ fostering a patient’s return to meaningful life roles.
Holistic Patient-Centered Care
Holistic care acknowledges the psychological impact of pelvic fractures‚ addressing anxiety‚ depression‚ and fear of re-injury alongside physical deficits.
Effective rehabilitation necessitates strong social support and considers the patient’s ability to return to work or daily activities.
Individualized treatment plans‚ respecting patient values and goals‚ are paramount for optimal recovery and long-term well-being.
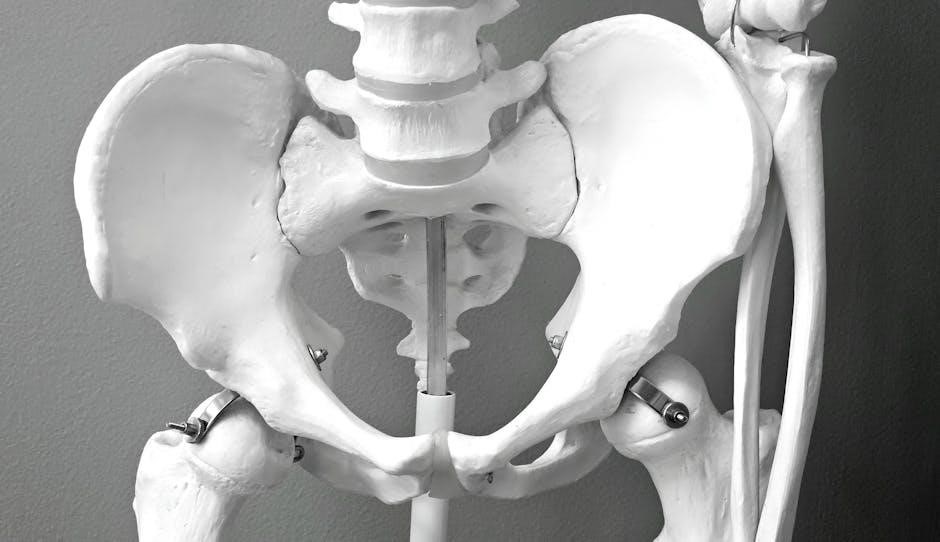
Radiological Assessment of Fracture Healing
Conventional radiology remains the primary method for evaluating fracture healing‚ particularly after surgical intervention‚ with timelines varying between 12-18 weeks.
Interpreting imaging results is vital for monitoring progress and adjusting the rehabilitation protocol accordingly.
Conventional Radiology Techniques
Conventional radiology‚ including X-rays‚ serves as a foundational tool for assessing pelvic fracture healing throughout the rehabilitation process. Serial radiographs allow clinicians to visualize callus formation and monitor fracture alignment.
These techniques are readily available and cost-effective‚ providing essential information regarding bone union and guiding adjustments to the protocol. Careful interpretation is key to tracking progress.
Interpreting Imaging Results
Interpreting radiographic findings requires careful attention to fracture line visibility‚ callus bridging‚ and overall bone density. Assessing for signs of non-union‚ such as persistent fracture lines or lack of callus‚ is crucial during rehabilitation.
Radiological evaluation informs protocol modifications‚ guiding progression or regression of exercises based on observed healing. Correlation with clinical findings is essential.

Sacroplasty and Internal Fixation Rehabilitation
Post-procedure precautions and modified rehabilitation protocols are essential following sacroplasty or internal fixation‚ typically requiring 12-18 weeks for healing.
Careful monitoring and gradual progression are key to optimizing recovery and preventing complications.
Post-Procedure Precautions
Following sacroplasty or internal fixation‚ initial precautions involve weight-bearing restrictions‚ often progressing from non-weight-bearing to partial‚ then full weight-bearing as tolerated.
Avoidance of excessive bending‚ twisting‚ and lifting is crucial to protect the healing fracture site. Pain management remains a priority‚ alongside diligent wound care.
Patients should adhere to activity modifications and attend scheduled follow-up appointments for radiographic assessment of fracture healing.
Modified Rehabilitation Protocols
Rehabilitation post-surgery‚ like internal fixation‚ typically requires a phased approach‚ often spanning 12-18 weeks for fracture healing.
Early phases emphasize gentle range of motion and isometric exercises‚ progressing to strengthening and gait training. Protocols are tailored based on fracture stability and individual patient factors.
Careful monitoring of healing via imaging guides progression‚ ensuring optimal loading and minimizing risk of non-union or hardware failure.
Potential Complications and Red Flags
Recognizing non-union signs and managing persistent pain are vital. Monitoring for complications like DVT is essential throughout the rehabilitation process.
Prompt intervention addresses issues‚ optimizing healing and preventing long-term functional limitations.
Recognizing Signs of Non-Union
Non-union presents with persistent pain at the fracture site‚ often exacerbated by activity‚ and a lack of radiographic healing progression over several weeks.
Clinical examination may reveal motion at the fracture site‚ indicating instability. Radiological assessment‚ including conventional X-rays‚ is crucial to confirm the absence of bridging callus formation‚ signaling delayed or absent healing.
Early identification allows for timely intervention‚ potentially requiring surgical revision.
Managing Persistent Pain
Persistent pain following pelvic fracture rehabilitation requires a multidisciplinary approach. Pharmacological interventions‚ including analgesics and neuropathic pain medications‚ may be necessary.
Physical therapy focusing on gentle range of motion‚ core stabilization‚ and proprioceptive training is vital. Addressing psychological factors‚ like anxiety and depression‚ is also crucial for effective pain management.
Consider referral to a pain specialist if symptoms remain refractory.

Long-Term Follow-Up and Outcomes
Long-term follow-up assesses functional outcomes and identifies potential issues. Preventing recurrence through continued exercise and fall prevention is essential for sustained well-being.
Assessing Functional Outcomes
Functional outcome assessment is vital post-pelvic fracture‚ evaluating a patient’s ability to perform daily activities. This includes gait analysis‚ range of motion measurements‚ and strength testing.
Standardized questionnaires and performance-based tests quantify improvements in mobility‚ balance‚ and overall physical function‚ guiding continued rehabilitation efforts and identifying any persistent limitations.
Preventing Recurrence
Recurrence prevention focuses on addressing underlying risk factors‚ particularly in fragility fractures. Fall prevention strategies‚ including home modifications and balance training‚ are essential.
Ongoing core strengthening and proprioceptive exercises enhance stability and reduce future fracture risk. Regular medical follow-up monitors bone health and adjusts interventions as needed.

Resources and Further Information
PubMed Central (PMC) offers extensive research on pelvic fracture rehabilitation‚ including scoping reviews and clinical guidelines. Access articles detailing treatment protocols and biopsychosocial approaches.
Professional organizations like the BOA provide standards of care. Focus Physiotherapy and similar clinics offer specialized rehabilitation programs. Explore resources for fragility fracture management.
